
Chronic Kidney Disease (CKD) Treatment
Chronic kidney disease (CKD) means that you have done permanent damage to your kidneys. Chronic means that the problem lasts a long time, and CKD can get worse over time. Most people with CKD don’t have any signs or symptoms until their kidneys are damaged. Blood and urine tests are used to figure out how badly the kidneys have been hurt. The level of creatinine in the blood can help tell how badly the kidneys are hurt.
In CKD, the damage to the kidneys is divided into 5 stages, from very mild damage in Stage 1 to kidney failure in Stage 5.
People with CKD can live normal, healthy lives if they make changes to their lifestyle and diet and take the right medicines for their condition.
Most damage to your kidneys lasts forever. Even though the damage can’t be fixed, there are things you can do, along with getting the right medical care, to keep your kidneys as healthy as possible for as long as possible. You might even be able to stop the damage from getting worse.

Hemodialysis
When the kidneys stop working, the dialysis process takes over their job of filtering the blood.
In the dialysis machine, the blood goes through a filter called a dialyser. This filter works like the kidney and removes waste and water from the blood. Hemodialysis is the name for this process.
Dr. Sourabh Gupta is an expert in planning dialysis, planning vascular access, and getting the most out of dialysis prescriptions. He thinks that people who are on dialysis should still live healthy, active lives.
He is an expert at planning advanced dialysis treatments for critical patients, like acute hemodialysis, Slow Low Efficiency Dialysis (SLED), and Continuous Renal Replacement Therapy (CRRT) for unstable patients in the intensive care unit or patients with very low blood.

Kidney Transplantation
Patients who have advanced kidney failure, which is defined as when the kidney function has been irreversibly reduced to 15% or less of its normal level, are candidates for kidney or renal transplant surgery.
A kidney from a donor is surgically implanted into the body of a recipient during a procedure known as a kidney transplant. The patient’s kidneys that are damaged are not removed unless it is medically necessary to do so under certain conditions.
Kidney transplants used to only be performed on patients whose blood groups were compatible with the donor. But thanks to recent developments in transplant science, it is now possible for people whose blood types do not match the recipient’s (known as ABO incompatible donors) to donate their kidneys.
Transplantation of the renal organs is Renal transplantation is Dr. Sourabh Gupta’s primary area of interest and where he excels professionally. He has worked in some of the country’s most prestigious transplant institutes for more than a decade, gaining experience in kidney transplantation there. He is an expert in the management of difficult transplant procedures that involve a high degree of risk, such as ABO incompatible renal transplants, second or third transplants, and sensitised transplants. He has experience performing transplants using both living related donors and deceased donors as well.
Kidney Biopsy
A kidney biopsy, also known as a renal biopsy, is the process of extracting one or more very small samples of kidney tissue and examining them under a microscope in order to look for any indications of disease or damage to the kidneys.
It is recommended to perform a kidney biopsy for one of the following reasons:
- To determine the cause of a possible kidney problem
- In order to determine the severity of a kidney condition
- To determine the likelihood of the kidneys being saved.
- In order to keep an eye on the patient’s treatment for kidney disease.
- In regard to a kidney transplant that is not functioning correctly
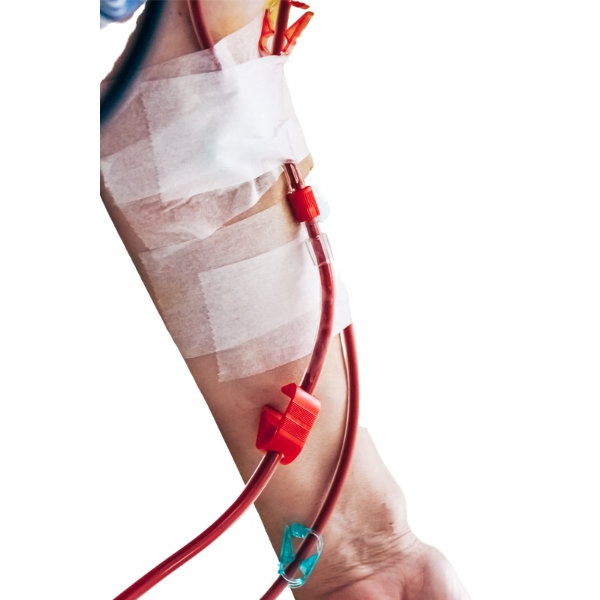
Vascular Access Planning
An access to a patient’s bloodstream, also known as a vascular access, is required before beginning treatment with hemodialysis. This access must be established first. The access enables the patient’s blood to be transported to and from the dialysis machine in a large volume and at a high speed, which facilitates the removal of toxins, waste, and excess fluid from the body of the patient.
There are two different kinds of vascular access used for dialysis:
- Temporary, in the form of catheters inserted into the patient’s legs and neck
- Permanent connections can be made using arteriovenous (AV) fistulas or AV grafts.
Patients who require routine hemodialysis are dependent on their vascular access for survival. In India, there are many patients who are unable to receive treatment because they do not have vascular access.
To ensure that the patient receives sufficient hemodialysis, Dr. Sourabh Gupta and his team perform careful and preventative planning for vascular access.
Hypertension
Hypertension, also known as high blood pressure, is the second leading cause of kidney failure after diabetes.
The majority of people who have hypertension don’t experience any symptoms at all. Over time, organs such as the eyes, heart, brain, and kidneys can become damaged due to hypertension, and this damage is frequently not recognised.
The majority of the time, hypertension can be managed with the appropriate medications, and further damage to organs can be avoided by receiving treatment at the appropriate time.
Dr. Sourabh Gupta is a leading authority on the diagnosis and treatment of a wide variety of hypertensive disorders and forms of high blood pressure. He is of the opinion that the best way to manage hypertension is to provide patients with sound advice in a variety of areas, such as diet, physical activity, and techniques for stress-free life management, in addition to prescribing medication.

Peritoneal Dialysis
During the process of peritoneal dialysis, a special cleansing fluid is inserted into the patient’s abdomen via a catheter. This catheter is called a peritoneal dialysis tube. The peritoneum, which lines the abdominal cavity, performs the function of a filter, removing waste products from the blood. After a predetermined amount of time, the fluid that contains the waste products that have been filtered flows out of the abdomen and is expelled. This treatment can be carried out anywhere, including at home, in the workplace, or even while travelling.
Dr. Sourabh Gupta is an expert in peritoneal dialysis and specialises in its planning and initiation. During the planning stage, a physician will insert a peritoneal dialysis catheter into the patient’s abdomen. During the initiation stage, the patient will begin the peritoneal dialysis procedure under the supervision of a medical professional. Finally, the patient and their family will receive training to perform the treatment on their own at home.

